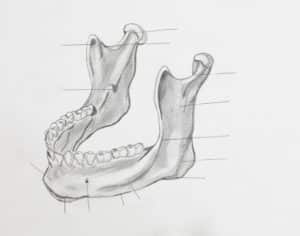
 TMJ is the acronym for temporomandibular joint. That’s a long complicated word for your jaw joint! If you want to find your jaw joint, put your fingers on the side of your face in front of your ears and open your mouth. The round, hard bone that you feel is your jaw joint. There is one on each side of your face and they are where your lower jaw connects to your skull. Your jaw joints allow you to talk, eat, chew, yawn, yell, sing, and more. TMD is the acronym for temporomandibular joint disorder which describes any problem you may have with your TMJs. The exact cause of TMD is difficult to diagnose.
TMJ is the acronym for temporomandibular joint. That’s a long complicated word for your jaw joint! If you want to find your jaw joint, put your fingers on the side of your face in front of your ears and open your mouth. The round, hard bone that you feel is your jaw joint. There is one on each side of your face and they are where your lower jaw connects to your skull. Your jaw joints allow you to talk, eat, chew, yawn, yell, sing, and more. TMD is the acronym for temporomandibular joint disorder which describes any problem you may have with your TMJs. The exact cause of TMD is difficult to diagnose.
Diagnosis
Unfortunately, it can be difficult to diagnose TMDs because the disorders vary widely, and people react to them differently. However, there are three main categories of TMDs:
- Myofascial pain: Pain or discomfort in the muscles that control the jaw.
- Internal derangement of the joint: This can describe a displaced disc, dislocated jaw, or injury to the condyle, often caused by trauma.
- Arthritis: A degenerative/inflammatory joint disorder that can affect your TMJ.
Diagnosis usually consists of taking a detailed medical and dental history; performing a thorough examination of the jaw, face, head, and neck; and a description of symptoms by the patient.
Symptoms
The following symptoms are often used to diagnose TMDs:
- Stiff and achy jaw muscles
- Headaches
- Neck pain
- Pain in the face and jaw
- Popping, clicking, or grating of the jaw joints
- Locking jaw, or limited jaw movement
- Malocclusion, or a change in occlusion (the way your upper and lower jaw fit together)
Treatment
Because most TMDs are difficult to diagnose, treatment is kept to a minimum and is non-invasive and conservative (treatment does not invade the jaw, face, or joint tissues, or involve surgery). Treatment can include:
- Therapy
- Night guard
- Pain meds
- Relaxation techniques
- Botox